Seren’s Perfect Home Birth
Born May 23, 2010 at 9:46 pm
7 lbs 10 oz, 13.5 inch head circumference , 20 inches long
 I think I knew I was going to be going into labor on Saturday night (May 22). I had just spent Friday and Saturday at the Colorado Midwives Association conference listening to the legendary Ina May Gaskin and when I got home I just felt like I needed to get the house ready. I was sort of irritable, flying around putting laundry away, etc. Kyle said, “Just do it tomorrow” but somehow I knew I should do it then. I had some sporadic contractions all Saturday evening (about 5-10 minutes apart but nothing serious), then had a glass of wine and went to bed.
I think I knew I was going to be going into labor on Saturday night (May 22). I had just spent Friday and Saturday at the Colorado Midwives Association conference listening to the legendary Ina May Gaskin and when I got home I just felt like I needed to get the house ready. I was sort of irritable, flying around putting laundry away, etc. Kyle said, “Just do it tomorrow” but somehow I knew I should do it then. I had some sporadic contractions all Saturday evening (about 5-10 minutes apart but nothing serious), then had a glass of wine and went to bed.
I continued to be woken by contractions all night long, some of them even working their way into my dreams! I had a dream we got pulled over by two cop cars for making an illegal U-turn. I was in the driver’s seat but somehow Kyle was driving. They asked me to step out of the car and I proceeded to have a contraction (in the dream and in real life) and squatted next to the car. The cops sort of backed away and said “Umm, never mind!”
I woke up around 7 am with contractions that were about 10 minutes apart and 1.5 minutes long. They were stronger than they had been and just weren’t going away. At that point I was thinking that I was maybe 75% sure I was going into labor. I got up to eat breakfast around 9 and as soon as I was upright they got a lot closer together (3-5 minutes) but still very manageable. I tried to eat some cereal but was kind of nauseous and gave up.
 Kyle took care of the girls while I spent some time in a lavender bath my friend Ashley had gotten me. They would slow down to about 10 minutes apart when I was laying down so I knew it was still early. I decided to take advantage of it and get some rest while I still could. I got out of the tub and laid down for about an hour. Haven came in to join me and we cuddled with her rubbing my back during my “belly squeezes.” It helped so much to see her sweet little face looking at me during the contractions! I just kept thinking that I was about to have a sweet little girl just like the one in front of me.
Kyle took care of the girls while I spent some time in a lavender bath my friend Ashley had gotten me. They would slow down to about 10 minutes apart when I was laying down so I knew it was still early. I decided to take advantage of it and get some rest while I still could. I got out of the tub and laid down for about an hour. Haven came in to join me and we cuddled with her rubbing my back during my “belly squeezes.” It helped so much to see her sweet little face looking at me during the contractions! I just kept thinking that I was about to have a sweet little girl just like the one in front of me.
I got up around 1:30 pm and Heather (one of my best friends) came over to hang out with Haven while Lyric took a nap and Kyle and I walked around the park by our house. It was a BEAUTIFUL day! Blue skies, warm but not hot, light breeze, perfect. We had a leisurely time walking around and swaying during contractions and talking. We definitely got some looks from neighbors! The only down side was that there was only one port-a-potty in the park and with Seren’s head so low I had to pee all the time. Whenever my bladder was full I’d have lots of contractions (about 2 minutes apart) which made walking to the potty really hard! Not to mention the ones I would have in the port-a-potty…
 Stacie (my midwife) and Miranda (my friend and doula sister) kept telling me that I didn’t have to keep walking if I didn’t feel up to it but it felt so good to be out in the sunshine. I even got a little bit of a sunburn during my labor which I think is fabulous! We walked around for about two and a half hours, just making loops and walking with one foot on the curb when I could. Sometimes we’d sit for a bit in the shade and update our birth team. Heather was the only one at our house yet so we were letting Stacie, Miranda, Jessica (our other midwife), Diane (one of my best friends), and Ashley (my friend and photographer) know where things were at. The contractions were (on average) 3 minutes apart while we were walking and sometimes spaced out to 5 minutes apart when we were sitting down, so I knew we were down to business but things were still early.
Stacie (my midwife) and Miranda (my friend and doula sister) kept telling me that I didn’t have to keep walking if I didn’t feel up to it but it felt so good to be out in the sunshine. I even got a little bit of a sunburn during my labor which I think is fabulous! We walked around for about two and a half hours, just making loops and walking with one foot on the curb when I could. Sometimes we’d sit for a bit in the shade and update our birth team. Heather was the only one at our house yet so we were letting Stacie, Miranda, Jessica (our other midwife), Diane (one of my best friends), and Ashley (my friend and photographer) know where things were at. The contractions were (on average) 3 minutes apart while we were walking and sometimes spaced out to 5 minutes apart when we were sitting down, so I knew we were down to business but things were still early.

Back from the park
At about 4:30 pm I started to feel like we should head back to the house. We got home and ordered some sandwiches from Jimmy John’s (the peppers were great until they weren’t). I could feel something switching over in my mind and body, and I felt like I wanted to start turning inward and go inside myself. I sat on the couch, Lyric in my lap, and breathed through some strong contractions.
Stacie came at 5:30 pm and I could feel things starting to move into active labor as I was rocking on the birth ball. The contractions were getting much more intense, much harder to relax into, and I started feeling sort of shaky. Stacie wanted to check me just once to try and figure out when to call Jessica, our second midwife. Seren’s head was so low in my pelvis it was hard for her to feel behind it and all the way around my cervix, but she told me that I was safely 5 cm, if not 6 or 7. This made me so happy! I was so worried I’d be 2 cm and be disappointed. I told myself I’d be satisfied with 4 cm and happy with 5 cm so this was perfect!
I decided I really wanted to get in the birth tub and I wanted Jessica and Miranda to come. I wanted to give Jessica a lot of time since she was driving up from Colorado Springs just for us! I think everyone got here exactly when they were meant to, even Ashley who flew in from Oklahoma at 6 pm and still made the birth!
 I got into the tub and have seriously never felt anything so wonderful!! The warm water washed over me relaxing all the muscles that I could relax and I felt like I could sink into the contractions so much easier! I labored in the tub while Jessica, Diane, and Miranda made their way here. Heather, Diane, and the kids played together outside and it was fun to hear their voices in the backyard. I think it was a good distraction for Haven and Lyric to have some friends to play with them. They came up periodically. Haven was particularly interested and wanted to hold me through some “belly squeezes.” Lyric came up and saw me have a contraction on the toilet and looked a little concerned, but when she saw everyone’s smiling faces (including mine) she seemed reassured.
I got into the tub and have seriously never felt anything so wonderful!! The warm water washed over me relaxing all the muscles that I could relax and I felt like I could sink into the contractions so much easier! I labored in the tub while Jessica, Diane, and Miranda made their way here. Heather, Diane, and the kids played together outside and it was fun to hear their voices in the backyard. I think it was a good distraction for Haven and Lyric to have some friends to play with them. They came up periodically. Haven was particularly interested and wanted to hold me through some “belly squeezes.” Lyric came up and saw me have a contraction on the toilet and looked a little concerned, but when she saw everyone’s smiling faces (including mine) she seemed reassured.
 I stayed in the tub most of the time, leaning on Kyle and moaning through contractions. Miranda was rubbing my back, and Stacie and Jessica would wipe my forehead and hold my hand if I needed them to. Everyone was perfectly in sync and were exactly what I needed! If one of them had to leave the room for something it felt like there was a definite void. The contractions were getting more intense and taking on a different quality. The contraction itself felt mostly muscular, but during the peak they started to take on a skeletal quality as well. I just felt like my whole pelvis felt sort of achy. This was different than my births with Haven and Lyric.
I stayed in the tub most of the time, leaning on Kyle and moaning through contractions. Miranda was rubbing my back, and Stacie and Jessica would wipe my forehead and hold my hand if I needed them to. Everyone was perfectly in sync and were exactly what I needed! If one of them had to leave the room for something it felt like there was a definite void. The contractions were getting more intense and taking on a different quality. The contraction itself felt mostly muscular, but during the peak they started to take on a skeletal quality as well. I just felt like my whole pelvis felt sort of achy. This was different than my births with Haven and Lyric.
 It turns out that this was because Seren was facing sunny side up. For those of you who don’t know, most babies come out OA (occiput anterior, or facing mom’s back). If a baby is OP (occiput posterior, or facing mom’s front) there is usually a greater surface area to the head and the back of the head pushes into mom’s sacrum causing what’s called “back labor.” Because I was carrying Seren totally different than Haven and Lyric (Seren’s back was always on the right, the girls were always on the left) this was my number one fear! I’ve been at births with women experiencing back labor that described it like an axe embedded in their back, even in between contractions. It can also cause a lot of false starts to labor, long labors, long pushing stages, etc.
It turns out that this was because Seren was facing sunny side up. For those of you who don’t know, most babies come out OA (occiput anterior, or facing mom’s back). If a baby is OP (occiput posterior, or facing mom’s front) there is usually a greater surface area to the head and the back of the head pushes into mom’s sacrum causing what’s called “back labor.” Because I was carrying Seren totally different than Haven and Lyric (Seren’s back was always on the right, the girls were always on the left) this was my number one fear! I’ve been at births with women experiencing back labor that described it like an axe embedded in their back, even in between contractions. It can also cause a lot of false starts to labor, long labors, long pushing stages, etc.
I didn’t want this to happen to me! The completely ironic thing was that I never had back labor. Besides the sort of aching in my pelvis it was completely normal! Not only that but it was by far my fastest birth! Apparently I have one of those pelvises that can accommodate an OP baby.
Around 8 pm things started to get really intense. The contractions were coming about every 3 minutes and it was getting more and more difficult to relax through them. In between, however, I was really able to relax and be present and happy about my baby being born that day. I asked to have some music played (Heart Sutra: Bliss and Serenity) and it just made me cry! It was the music that was playing at our wedding and at Lyric’s birth, and it made me think of when my last sweet baby was born.
 I was starting to think that this intensity was going to last forever. I had only been checked once (I had GBS, group B strep, in my urine and everyone agreed on keeping vaginal exams to a minimum) and I had no idea how close I was to giving birth. I also had never lost any of my mucous plug or had any bloody show, the usual signs that you’re getting closer. I was starting to think I couldn’t do it. Jessica said, “Don’t worry, she’s just packing up her womb” which made me laugh.
I was starting to think that this intensity was going to last forever. I had only been checked once (I had GBS, group B strep, in my urine and everyone agreed on keeping vaginal exams to a minimum) and I had no idea how close I was to giving birth. I also had never lost any of my mucous plug or had any bloody show, the usual signs that you’re getting closer. I was starting to think I couldn’t do it. Jessica said, “Don’t worry, she’s just packing up her womb” which made me laugh.
And then everything happened at once, LITERALLY! I felt a huge gush as my water broke like a torrent. I immediately started projectile vomiting (on Kyle, sorry babe!), and as soon as that subsided I felt her stretching my perineum. I shouted, “She’s coming NOW, go get Haven!” and that was all I could muster before my body took over and started to bear down. It was the most amazing, crazy, beautiful, frightening thing I’ve ever felt! Haven’s pushing and birth had been very coached (first baby, epidural) and even though I waited for a while with Lyric I never had that urge to push. This was completely different. My body took over and it was like I was hanging on by my fingernails! Jessica told me later, “It’s like throwing up except it’s throwing down,” which is exactly how it felt! I’d never realized how strong the fetal ejection reflex is.
 Kyle jumped in the tub to catch Seren like we planned (in his clothes, there was no time to put on a swimsuit) and Haven did as well. A few minutes later Seren’s head was born, it whipped around like a corkscrew, then shoulders, and then she was out. I couldn’t believe how aware I was of every sensation. I could feel every contour of her body as she came out and there was such a relief once she was out. I had really wanted not to tear with this one like I did with the others and had told everyone prenatally that I wanted reminders to go slowly, stretch, breathe her out, etc. Now everything was happening so fast that I felt like my my mind was telling my body “Slowly, breathe!” and my body was saying, “Nope, here we go, out she comes!” Even so, Stacie told me later that my body eased her out beautifully, that it took breaks when it should have to let her rotate, that I stretched wonderfully, etc. In fact I didn’t need stitches after all! I only had a “skid mark” that would heal if I rested enough postpartum.
Kyle jumped in the tub to catch Seren like we planned (in his clothes, there was no time to put on a swimsuit) and Haven did as well. A few minutes later Seren’s head was born, it whipped around like a corkscrew, then shoulders, and then she was out. I couldn’t believe how aware I was of every sensation. I could feel every contour of her body as she came out and there was such a relief once she was out. I had really wanted not to tear with this one like I did with the others and had told everyone prenatally that I wanted reminders to go slowly, stretch, breathe her out, etc. Now everything was happening so fast that I felt like my my mind was telling my body “Slowly, breathe!” and my body was saying, “Nope, here we go, out she comes!” Even so, Stacie told me later that my body eased her out beautifully, that it took breaks when it should have to let her rotate, that I stretched wonderfully, etc. In fact I didn’t need stitches after all! I only had a “skid mark” that would heal if I rested enough postpartum.
 From my water breaking to Seren coming out was just 6 MINUTES! At this point Lyric was upstairs as well. We had tried to get her up here for the birth but everything happened so fast there just wasn’t a good opportunity. She jumped in the tub with us and started blowing bubbles in the birth water (oh well)! The girls took turns smooching Seren’s head and Lyric kept pointing to her saying “Baby, nursing!” though quizzically looking at my empty belly.
From my water breaking to Seren coming out was just 6 MINUTES! At this point Lyric was upstairs as well. We had tried to get her up here for the birth but everything happened so fast there just wasn’t a good opportunity. She jumped in the tub with us and started blowing bubbles in the birth water (oh well)! The girls took turns smooching Seren’s head and Lyric kept pointing to her saying “Baby, nursing!” though quizzically looking at my empty belly.
 We all looked our new baby over. No one could get over the fact that she was such a pretty baby! So perfect and chubby with a button nose and sweet little rosebud lips and a little round head. She reminded me a lot of Haven, especially the nose.
We all looked our new baby over. No one could get over the fact that she was such a pretty baby! So perfect and chubby with a button nose and sweet little rosebud lips and a little round head. She reminded me a lot of Haven, especially the nose.
Since she came out so fast Seren was a little stunned. Her APGARs were 8-8 (off for color and tone) but her respirations and heart rate were as perfect as it had been during labor. A little postural drainage from Jessica helped her get some of the gunk out and then she pinked up quite nicely (no bulb syringes at this birth thank you very much!). Kyle felt that the cord was still pulsing so we knew that she was still getting lots of oxygen from the placenta. About 25 minutes later Seren latched on (and I got a dose of Angelica herb), and I felt cramping and pressure, as well as a little separation gush of blood. Then I pushed out the placenta. All in all I only lost 250 cc’s of blood, which is really great!
 We decided to go and get cozy on the bed as a new family. Seren kept nursing like a champ. After a long while of that I got up to try and pee and Kyle took Seren for a while. He was such a sweet daddy, smooching and loving on her. He had waited for a long time to hold an itty bitty baby.
We decided to go and get cozy on the bed as a new family. Seren kept nursing like a champ. After a long while of that I got up to try and pee and Kyle took Seren for a while. He was such a sweet daddy, smooching and loving on her. He had waited for a long time to hold an itty bitty baby.

Haven cutting Seren's cord
I came back and we did the newborn exam and of course she was perfect, term, and healthy! Stacie helped Haven to cut the cord like she had been telling her preschool teachers for months. Then Haven got to hold her (Kyle had to put Lyric to bed, she was so tired) and Miranda made placenta prints which turned out beautiful. I was feeling great and Seren was nursing and pink and beautiful when everyone went home. In fact, Seren nursed until 2:30 am when I finally cut her off and gave her my pinkie finger so I could get some sleep. She’s still a champion nurser.
It was by far the most perfect, lovely, empowering, beautiful birth I could have ever hoped for! I absolutely loved giving birth in my own home because I could settle into my space and my body and it made everything really peaceful and manageable. I wouldn’t do it any other way!


Our midwife Stacie Meredith

Haven holding her sister


 I just got the best sibling prep book for any sibling and/or parent who is interested in attending a birth.
I just got the best sibling prep book for any sibling and/or parent who is interested in attending a birth.  Here is a synopsis for the book:
Here is a synopsis for the book: Here is a synopsis for the dvd:
Here is a synopsis for the dvd:


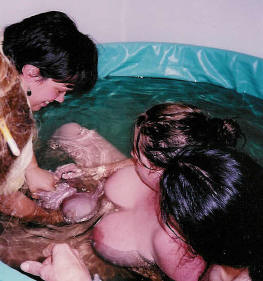 A midwife should have the same screening criteria as a doctor screening for risk factors. Depending on licensing status, some midwives must refer to a physician for cases of breech or twins or even VBAC. Other states have less restrictive or no guidelines. This must be discussed.
A midwife should have the same screening criteria as a doctor screening for risk factors. Depending on licensing status, some midwives must refer to a physician for cases of breech or twins or even VBAC. Other states have less restrictive or no guidelines. This must be discussed.


 Can I stay in the water to birth my baby?
Can I stay in the water to birth my baby? Here is a place where you can post comments about what you wish you had known going into birth.
Here is a place where you can post comments about what you wish you had known going into birth. Massage can be a great way to help a laboring woman cope with labor. During contractions a woman may tense up her muscles leading to the fear-tension-pain cycle which can easily spiral out of control. Massage helps a woman relax as well as helps to keep her mind off the painful sensations. Massage can also release endorphins which help the mom cope with pain. Here are some types of massage that some women find helpful. Don’t be discouraged if in labor she rejects these! What might feel good one moment might feel horrible the next!
Massage can be a great way to help a laboring woman cope with labor. During contractions a woman may tense up her muscles leading to the fear-tension-pain cycle which can easily spiral out of control. Massage helps a woman relax as well as helps to keep her mind off the painful sensations. Massage can also release endorphins which help the mom cope with pain. Here are some types of massage that some women find helpful. Don’t be discouraged if in labor she rejects these! What might feel good one moment might feel horrible the next!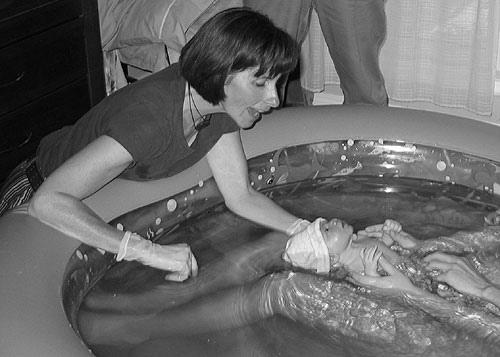 The Midwives Model of Care reflect the idea that pregnancy, birth, and postpartum are a natural, normal phase in a woman’s life and should not be treated like a catastrophe waiting to happen. They protect the birthing space from elements that might make a mother self-conscious or alarmed. They also discourage medical management of labor and instead let the process work while lovingly guiding the laboring woman emotionally, physically, and spiritually.
The Midwives Model of Care reflect the idea that pregnancy, birth, and postpartum are a natural, normal phase in a woman’s life and should not be treated like a catastrophe waiting to happen. They protect the birthing space from elements that might make a mother self-conscious or alarmed. They also discourage medical management of labor and instead let the process work while lovingly guiding the laboring woman emotionally, physically, and spiritually.